Beta Thalassemia Major
What is Beta Thalassemia Major?
Beta Thalassemia Major is the most prevalent of all the Thalassemias in India. It is estimated that there are nearly 100,000 persons with Thalassemia Major in India and around 35-40 million carriers. Beta Thalassemia Major is the most severe form the spectrum of Beta Thalassemias with the thalassemia trait or minor being only carriers with only mild anemia or even normal hemoglobin levels and Thalassemia Intermedia patients being less severely anemia than Thalassemia Major and requiring start of transfusions at a later age than children with Thalassemia Major. In Thalassemia Major, the severe anemia is due to the defective red blood cells which have a reduced life span. A person with Beta Thalassemia Major is completely transfusion dependent from about 6-24 months of age requiring 2-4 units of blood every 15-30 days for survival apart from complex iron chelation to control the excess iron deposition due to the repeated blood transfusions and increased iron absorption caused by this ineffective red blood cell production.
According to WHO estimates, around 1.1% of couples globally are at a risk of having children with one of the hemoglobin disorders. Prevalence is estimated at 2.77 per 1000. Of the 332000 global annual births of hemoglobin disorders, around 56,000 are affected by Beta Thalassemia Major.
Patterns of Inheritance
The Thalassemias are inherited in an autosomal recessive pattern which means both the mother and father have to be carriers of Beta Thalassemia for the child to present with Beta Thalassemia Major. Heterozygous carriers or minors with one copy of the thalassemia trait gene have no symptoms whereas a child/adult with homozygous thalassemia will present with the disease.
When both parents are carriers of the Beta Thalassemia trait, there is a 25% chance that every offspring will present with homozygous Beta Thalassemia Major with transfusion dependency. Beta Thalassemia is caused by a mutation in the HBB gene. The HBB gene encodes the β-chain and is located on chromosome 11.

Image source: Pixabay
Symptoms and Diagnosis
Symptoms
Babies with Beta Thalassemia Major usually present with symptoms from the age of 2-3 months. Check for the following symptoms in your baby if you think he/she may have Beta Thalassemia Major:
- Baby is pale and lethargic and does not suckle adequately
- Baby is frequently coming down with infections like fever, vomiting and diarrhoea
- Baby fails to grow
If your baby has any of the above symptoms, please see your paediatrician immediately. He/she will refer you to a hematologist to confirm the diagnosis.
In order to compensate for the anemia, the liver and spleen increase in size and the bone marrow in all the bones including the skull and face bones and long bones tries to make blood. However, since this is ineffective red blood cells the person continues to have anemia and develops bone thinning and facial abnormalities. Blood transfusions are essential to treat the severe anemia. If severe anemia is left untreated it can lead to heart failure. Life-long blood transfusions of packed red blood cells to keep the hemoglobin above 9g/dl is required to prevent deformity and enlargement of the spleen which is a result of inadequate blood transfusions. If you see signs and symptoms of Thalassemia, do not hesitate to approach a pediatrician who will help you get a diagnosis.
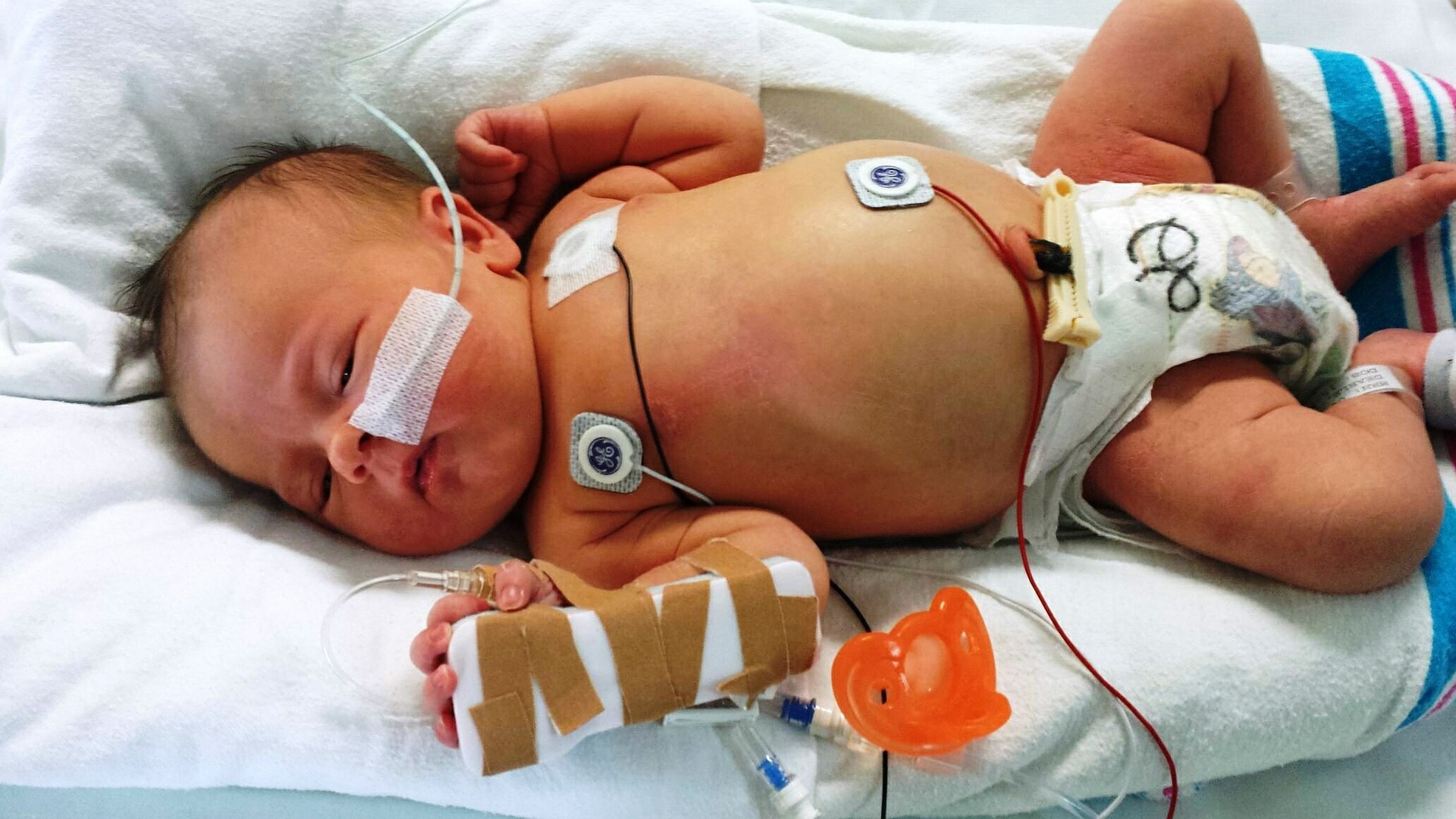
Image source: Pixabay
Diagnosis
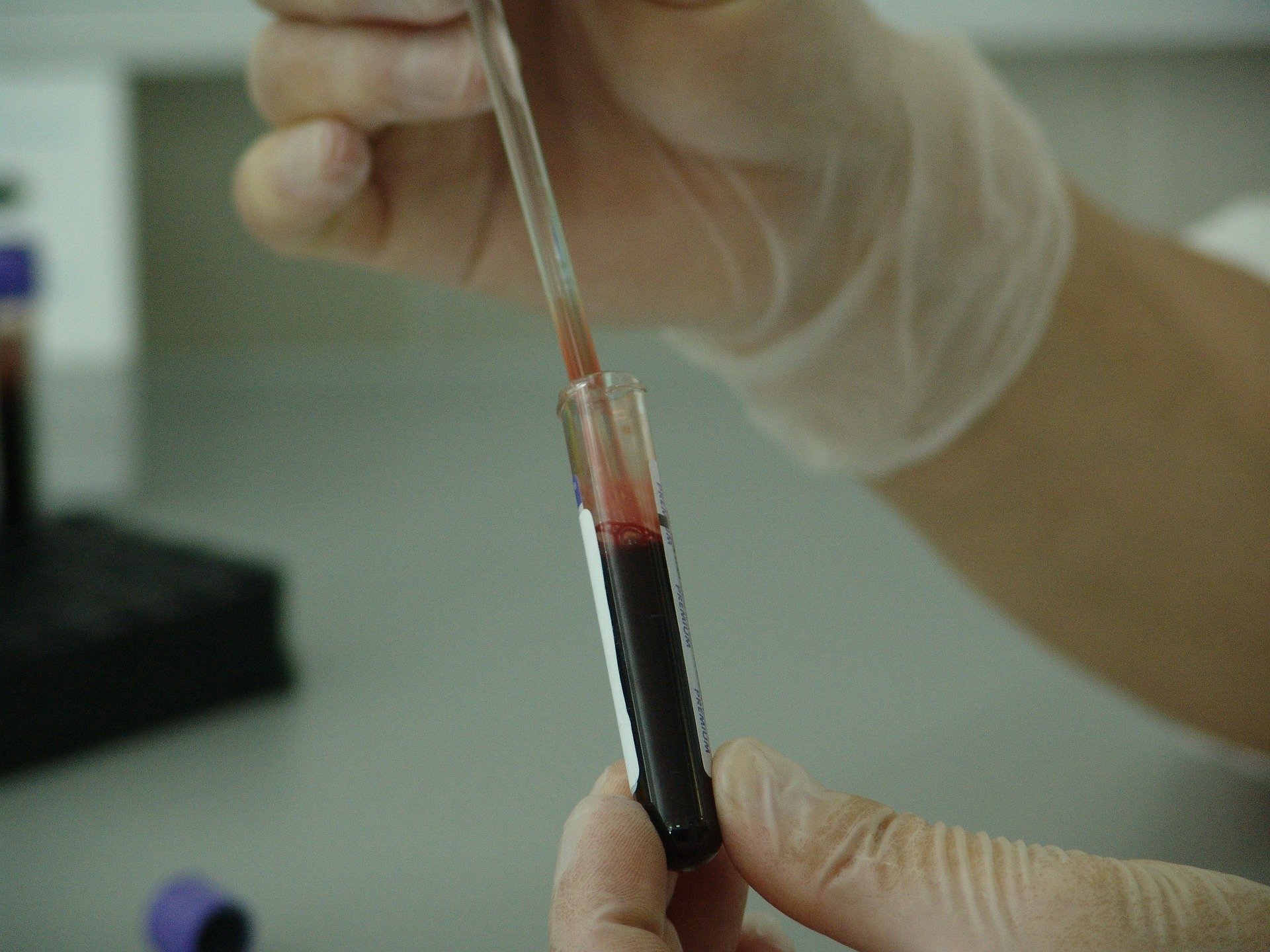
If your pediatrician suspects Thalassemia, he/she will do some simple blood tests to confirm. Some of the blood tests include:
- Complete Blood Count (CBC) which usually indicates hemolytic anemia with increased WBCs (white blood cell counts) and microcytic anemia in children with a big spleen lower numbers of platelet count may be seen
- High-performance liquid chromatography (HPLC) and capillary zone electrophoresis (CE) system can distinguish Thalassemia Major and the carriers. Iron studies usually indicate high serum iron concentration because of increased iron absorption from the intestine/gut
Up to now, more than 1,800 mutations causing hemoglobinopathies have been discovered. These mutated α and β globin genes in different combinations lead to over 60 thalassemic diseases.
The above tests suffice to get an initial diagnosis of Beta Thalassemia Major if the child has not received any blood transfusion before the blood sample has been taken. If the child has already had a blood transfusion then blood tests of the parents may help in making the diagnosis.
DNA testing for the child and parents is recommended to confirm the genotyping of the family. This is useful if the couple want to have more children, they should be advised prenatal testing of the next child as with each pregnancy they have a 25% risk of having a child with Beta Thalassemia Major. Though they have a 75% chance of having a child who has only thalassemia trait or is normal, this risk can be made close to zero with prenatal testing. This healthy sibling if he/she is a HLA-match for their Beta Thalassemia child (bone marrow transplant). DNA analysis is also absolutely necessary for prenatal testing.

Image source: Pixabay
Current Management
- Blood transfusions - Thalassemia Major and some Thalassemia Intermedia patients require lifelong treatment in the form of regular blood transfusions to treat the severe anemia, promote growth and normal development. Children/adults with Thalassemia Major usually require 1-2 units of blood every 15 -21 days.
- Iron chelation - Apart from regular blood transfusions, iron chelation therapy in the form of deferoxamine (desferal) subcutaneous infusion (with a pump), oral tablets like deferiprone (kelfer), deferasirox (few common brands are asunra, desirox, defrijet or oleptiss) is required as the excess iron from blood transfusions accumulate in the vital organs causing severe damage and even death due to cardiac and liver failure. Good iron chelation therapy prolongs life and decreases the complications caused by the iron overload on other organs like endocrine glands, bones and joints.
- Your hematologist will be the best person to advise you on the optimal mode of iron chelation, regular monitoring of serum ferritin and other tests to check that the heart, liver and other organs are working properly. Most thalassemia centers will guide you on these necessary requirements.
- Sometimes combination of iron chelation may be needed in some patients if one iron chelation medicine does not work. Please note that all medicines have side effects. It is advisable to take medicines as recommended by the doctor and get all the prescribed monitoring tests done. You need to keep your doctor informed if you experience side effects like joint pain, nausea, vomiting, gastric trouble or any other uneasiness. If you are on iron chelation medicines like oral tablet/dispersible tablets or subcutaneous (skin) injections, you will need to regularly (every 3 months) test for complete blood counts, liver and kidney function. You will need a blood test for serum ferritin (to measure blood iron concentration) every 3-6 months to see if your iron chelation medicines are adequately controlling the iron levels. Very high iron levels can cause damage to the heart and liver.
- A T2*STAR MRI is useful in children over the age of 10 years to check for iron overload in the vital organs – heart and liver. Sometimes the iron levels in the heart and liver may not co-relate with the serum ferritin. Finding iron overload in these organs allows the doctors to change iron chelation medicine.
- Regular supplements and medications - your doctor may put you on some supplements like folic acid, calcium, vitamin D, vitamin C and vitamin B12. It is advisable not to take any extra tablets or supplements without first consulting your doctor. You should not take any medicines containing iron.
- Diet and exercise - people with Thalassemia can lead a fairly normal life if transfused regularly and compliant with iron chelation Exercise is important to keep the bones healthy as iron affects the bones. People with Thalassemia can safely go for long walks, light jogging, floor exercises, swimming and dancing. Gym maybe permitted by the doctor with proper training from a gym instructor. People with Thalassemia need to be on a low-iron diet avoiding iron-rich foods like finger millet (ragi), red meat and soyabeans. Taking tea with meals is also a good way of decreasing iron absorption.
As of today, bone marrow transplant is the only cure for thalassemia. A full HLA match with a sibling or unrelated donor is recommended preferably before the age of 12. The child must be well-maintained with regular transfusion, iron chelation and free from infections like hepatitis B and C. Your doctor will advise you on the procedure for bone marrow transplant.
Curative Therapies
As of today, bone marrow transplant is the only cure for Thalassemia. A full HLA match with a sibling or unrelated donor is recommended preferably before the age of 10 years. The child must be well-monitored and receive regular transfusion, iron chelation and be free from infections like hepatitis B and C. Your doctor will advise you on the procedure for bone marrow transplant. There is Government support for this procedure if the child has a HLA matched brother or sister and the child with Thalassemia Major fits the above criteria.
Newer Therapies
New medicines like Luspatercept-AAMT are recently approved by the US Food and Drug Administration (USFDA) and European Medicines Agency (EMA) and may increase the hemoglobin and thereby decrease the number of transfusions needed. The best results are seen in Thalassemia Intermedia patients, but some thalassemia major patients may also benefit. It is important to remember that long term safety of many medicines have not been tested in patients and are not yet considered standard of care.
Investigational Therapies
Currently gene therapy is being studied as a permanent cure for Beta Thalassemia Major. Gene therapy involves replacing the defective gene with a normal gene through the help of load carrying viral vectors. The normal gene will be able to produce sufficient quantities of the hemoglobin to enable the patient lead a normal life without transfusion dependency.
Currently Boston-based Bluebird bio is the first company in the world to get a conditional market approval for their Beta Thalassemia gene therapy called Zynteglo®. It is the world’s first gene therapy for people above 12 years of age to cure Beta Thalassemia Major.
Gene editing techniques are also being studied and explored as a permanent cure for Beta Thalassemia. This involves reactivating the gene responsible for fetal hemoglobin production, BCLA11. After collecting blood stem cells from the patient, it is edited to reactivate the production of fetal hemoglobin and then infused back into the patient. Increasing the fetal hemoglobin levels boosts blood production and removes the need for transfusion dependency thereby curing the patient.
You can learn more about gene editing trials at https://clinicaltrials.gov/ct2/show/NCT03432364
References
Description, Types, Causes, Diagnosis, Treatment
https://patient.info/doctor/thalassaemia-pro#nav-4
http://www.thalassemia.org/learn-about-thalassemia/about-thalassemia/
http://thalassemia.com/genetics-trait-testing.aspx#gsc.tab=0
https://www.mayoclinic.org/diseases-conditions/thalassemia/diagnosis-treatment/drc-20355001
Etiology
https://thalassemia.com/genetics-inheritance.aspx#gsc.tab=0
https://rarediseases.info.nih.gov/diseases/871/beta-thalassemia
https://www.ncbi.nlm.nih.gov/books/NBK22200/
Epidemiology
https://www.who.int/bulletin/volumes/86/6/06-036673/en/
Gene Therapy
https://www.labiotech.eu/gene-cell-therapy/bluebird-bio-zynteglo-gene-therapy/
Standard of care guidelines
Children’s Hospital and Research Center Oakland
https://thalassemia.com/SOCGuidelines2012.pdf
United Kingdom Thalassaemia Society
https://ukts.org/wp-content/uploads/2019/12/Standards-2016final.pdf
National Health Mission India
https://nhm.gov.in//NHM_Hemoglobi.pdf
Thalassaemia International Federation
https://www.resonancehealth.com/clinician-information/Thalassaemia.pdf
National Resources
New Delhi
Thalassemics India
Address:
A9, Nizamuddin West,
New Delhi - 110013
Phone: 011 41827334, 46595811 or 9810019950
Email - thalassemicsindia@gmail.com
Website - http://www.thalassemicsindia.org/index.php
National Thalassemia Welfare Society
Address:
KG 1/97, Vikas Puri,
New Delhi-110018
Phone 011-25507483, 25511795 or 9311166710,711,712
Website - http://www.thalassemiaindia.org/Default.aspx
Disease Videos
Beta Thalassemia - causes, symptoms, diagnosis, treatment, pathology
Alpha-thalassemia - causes, symptoms, diagnosis, treatment, pathology
What is thalassemia
Reimaging beta-thalassemia and its treatment
All about thalassaemia
Keywords
Beta Thalassemia Major, Hemoglobin, Carriers, Minors, Trait, HBB Gene, Bone Marrow Transplant (BMT), HLA-Match, Blood Transfusion, Iron Chelation, Serum Ferritin, Deferoxamine, Deferasirox, Deferiprone, Gene Therapy, Gene Editing, Foetal Hemoglobin, BCLA11 Gene